Aligning the Exposome and Health Equity with Brain Aging amidst a Changing Climate
What am I reading? Aligning the Exposome and Health Equity with Brain Aging amidst a Changing Climate
If you’re interested in contributing a short What Am I Reading post, we’d love to hear from you! Email us at cache@colorado.edu.
Written by Kelly Perry and Jenna Merenstein
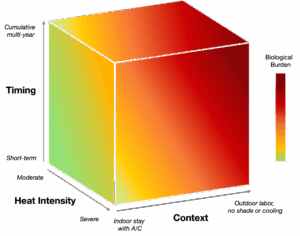
When people think about brain health and aging, they might first think about the role of genetics or lifestyle factors. Both factors are important, though a growing body of research shows something else is also playing a major role in shaping how our brains age: the physical, social, and structural exposures we experience across our lives—from before birth through older age. Scientists refer to this as the exposome, and understanding it is key to addressing cognitive decline in a changing climate (Li et al 2025). In our recent Alzheimer’s & Dementia Perspective, we argued that understanding both healthy aging and Alzheimer’s disease and related dementias (ADRDs) requires an exposome- and equity-centered lens that considers the environmental and social conditions (including systemic inequities and systems-level resilience strategies) that shape brain health. We include the framework introduced in our paper in Figure 1.

Figure 1. An equity- and justice-centered framework for linking the exposome and neurocognitive health across the life course (from Perry KE & Merenstein J, 2026)
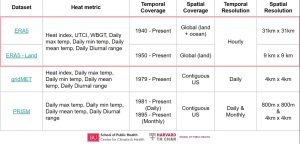
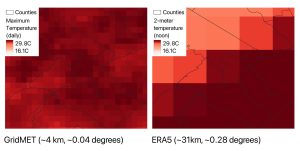
A recent Nature Medicine paper by Legaz et al. titled “The Exposome of Brain Aging across 34 Countries,” provides a compelling example of how this framework can be applied in practice. The authors examined 73 physical and social exposomal factors (e.g., air pollution, temperature, greenspace, gender equality, democracy, and access to drinking water) and their relation to neuroimaging measures of brain structure and brain function for 18,701 participants that varied in cognitive status (cognitively normal, mild cognitive impairment, Alzheimer’s disease, and frontotemporal lobar degeneration). Participants were recruited from 34 countries across Latin America, North America, Europe, Asia, Africa, and Oceania, thereby helping address the systemic underrepresentation of low- and middle-income countries (LMICs) in neuroimaging research.
Legaz et al. demonstrated that aggregated exposome models explained significantly more variance in brain aging than any single exposure alone—up to 15.5 times more than individual factors. Furthermore, their results highlight the impact that structural inequities embedded within neighborhoods, institutions, and political systems have on brain aging: physical exposures (e.g., higher air pollution, reduced greenspace, and extreme temperatures) were strongly associated with accelerated structural brain aging. In contrast, social exposures (e.g., poverty, weaker rule of law, and decreased civic participation) were associated with accelerated functional brain aging. The latter was shown to be especially true for female participants in the study, where reduced rights-related factors and poor soil and water quality predicted accelerated aging in females more than males. Their findings underscore a central argument of our Perspective: that environmental neuroscience needs to overcome the siloed approaches that are traditional hallmarks of the discipline, e.g., focusing on a single exposure or a single high-income country cohort.
Tools such as the Area Deprivation Index (ADI) and the Neighborhood Atlas are helpful in elucidating these structural, systemic inequities that adversely impact brain aging and increase the risk of ADRDs. While Legaz et al. used country-level indicators, neighborhood-level metrics such as ADI can provide finer resolution for studying how disadvantage shapes brain health within countries and across communities. ADI captures social dimensions such as income, education, employment, and housing quality, allowing researchers to better characterize cumulative disadvantage at the local scale. Similarly, the Neighborhood Atlas (which hosts the ADI) provides standardized geospatial measures of neighborhood deprivation that can be linked to neuroimaging, cognition, and dementia outcomes (Hunt et al 2020; Kim et al 2024). These tools help operationalize the “social exposome” by connecting place-based inequities to measurable differences in brain structure and function.
Building better data in this field also means improving access to neuroimaging itself. As we discussed in our Perspective, one major barrier to exposome- and equity-informed neuroscience is that advanced MRI remains inaccessible in many under-resourced and rural settings. Emerging low-field MRI initiatives, including recent work at Cardiff University, are helping address this gap by developing lower-cost, portable systems capable of whole-brain imaging. These efforts are particularly important for LMICs, where the burden of environmental exposures is often highest but access to imaging infrastructure is lowest. Legaz et al.’s multi-country study underscores why this matters: without broader imaging access, we risk building evidence only from the least exposed populations.
Protecting brain health equitably requires shifting toward prevention and systems change. Policies that promote cleaner air and water, safer housing, and equitable urban design can reduce harmful exposures across the life course. Investments in expanding access to green spaces, pollution control, and community infrastructure benefit physical health and cognitive resilience. Legaz et al.’s study provides strong empirical support for the notion that environmental and social conditions fundamentally shape brain aging outcomes. As climate change intensifies these exposures globally, building inclusive datasets (e.g., The Neighborhood Atlas), improving access to neuroimaging (e.g., investing in low-field scanners), and centering health equity in brain health research and policy will be essential for ensuring healthy cognitive aging for communities worldwide.